Traumatic Brain Injuries in the Veteran Community
My client was unable to look me in the eyes all of a sudden, and although he had been chatty moments before, he was painfully quiet now. Over the past few days, my client’s mood swings had become increasingly more extreme. He had told me he’d been unable to sleep for 6 nights in a row and that his insomnia had been intensifying his anxiety and depression. He suffered from a traumatic brain injury (TBI) and post traumatic stress disorder (PTSD), which had both been a result of a severe accident while serving in Afghanistan. The effects of the accident still plagued him in his 40’s. He found himself unable to focus on conversations–especially at work. He was a homeless veteran trying to battle his TBI and PTSD without medical help.
My client’s experience is a tragic one, but not entirely uncommon. From 2000 to 2021, more than 450,000 U.S. service members were diagnosed with a TBI. When TBIs are paired with PTSD, which is usually the case for veterans, the two seem to reinforce each other. In fact, clinical outcomes have shown that a traumatic brain injury can impede recovery from psychological trauma. Without understanding these conditions and seeking help, they can lead to difficulties in maintaining relationships, jobs and a healthy home life.

Army Medical Center in Honolulu educates soldiers on TBI during Brain Injury Awareness Month.
Mild Traumatic Brain Injuries
Of the nearly half a million TBIs in the veteran community, the majority are categorized as mild (mTBIs). These types of injuries are also referred to as concussions, and the symptoms usually resolve themselves within days or weeks. Vehicle crashes, sports-related injuries and explosion impacts from military service are the leading causes of mTBIs. In each of these situations, violent movement causes the brain to smash into the skull. This results in temporary inflammation and swelling inside the brain, which disrupts normal brain function.
Symptoms of mTBI can range anywhere from headaches, blurry vision, and nausea to difficulty speaking, memory problems and ringing in the ears. Researchers are still trying to explore the long-term effects though, as some individuals experience mTBI symptoms that persist for several months or longer.

Effects of shell shock on Private Sheehan (left) at the first aid station in Courboin, France.
For U.S. forces deployed to Afghanistan and Iraq, blast exposure is the leading cause of mTBI. However, mild traumatic brain injuries are not just modern-day phenomena. The evidence for mTBI dates all the way back to WWI when explosives first made their debut on the battlefield. Soldiers who had experienced frequent bouts of explosive artillery fire developed shell shock or “commotio cerebri.” Men reported migraines, amnesia, insomnia, difficulty concentrating, depression and even suicidality. These symptoms perfectly match those reported by the current veteran community.
Moderate and Severe Traumatic Brain Injuries
Moderate and severe TBIs are caused by direct blows to the head or penetrations to the skull. Falls, firearm-related injuries, car crashes and assaults lead to most moderate and severe TBIs. In the veteran community, bullets and shrapnel puncturing the head are common causes of severe TBI. When these foreign objects penetrate the skull at high speed, they create bleeding, bruising or torn tissues within the brain.
Although moderate TBI and severe TBI are very similar, there are ways in which they differ. In cases of moderate traumatic brain injury, loss of consciousness for less than 24 hours is possible, but not guaranteed. However, someone with a severe traumatic brain injury always experiences an extended loss of consciousness or a coma. Additionally, medical staff may keep an individual with a moderate TBI under observation for a short time, whereas a person with a severe TBI usually requires extensive surgery and follow-up.
In some cases though, recovery is not an option. Severe traumatic brain injuries can lead to vegetative states, deadly strokes or life-threatening blood clots.
Symptoms
Even after surviving a moderate or severe TBI, researchers estimate that a person’s life expectancy is 9 years shorter. This is because TBIs increase the risk of getting seizures, infections and pneumonia down the road. Other lifelong symptoms include slurred speech, loss of vision, constant numbness or tingling of limbs, increased confusion or restlessness and loss of coordination.
Many individuals report significant emotional and behavioral changes in addition to the physical symptoms that accompany TBI. 29% of those suffering from moderate or severe TBI report being unsatisfied with life. 33% rely on others for help with everyday activities, and 55% do not have a job (but were employed at the time of their injury). It’s clear from these statistics that TBIs can drastically change an individual’s mental, emotional and physical health. Although these injuries happen almost instantaneously, their impacts last a lifetime.
The Effects of Multiple TBIs
Just as TBI and PTSD interact with each other to reinforce symptoms, multiple TBIs over time can compound an individual’s lifelong symptoms. Researchers have found that Iraq and Afghanistan veterans who suffered multiple traumatic brain injuries were about twice as likely to report recent suicidal ideation than vets with no TBI or vets with just one TBI. A history of these injuries seems to exacerbate mood problems, changes in personality and difficulties in controlling impulses.
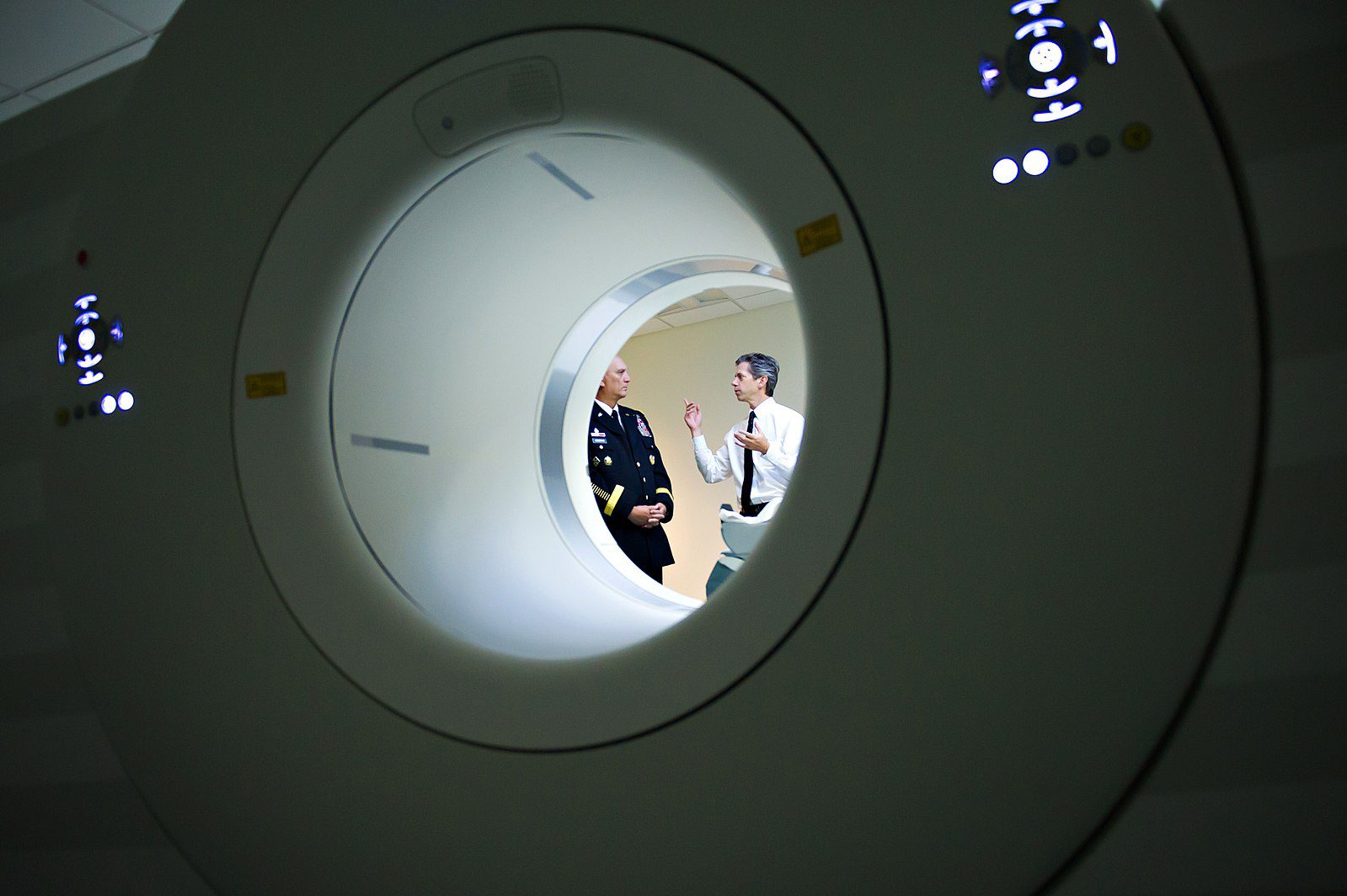
U.S. Army Gen. Raymond T. Odierno, left, listens to a research physiologist describe the measures Walter Reed National Military Medical Center takes in treating TBI.
How to Cope
Although it seems like it would be an obvious condition to spot, not everyone realizes they have a TBI–even when the symptoms are chronic. These injuries can be tough to identify, as there may not always be visible wounds that accompany them. Additionally, the symptoms of a traumatic brain injury are similar to those of PTSD, which means it’s difficult for medical practitioners to separate one from the other. TBIs can hide in plain sight, and without treatment, they can negatively impact an individual’s ability to maintain relationships, jobs and healthy habits.
In some cases, rehabilitation will be necessary to improve one’s ability to function at home and in the community. After recovery in a hospital setting, veterans should seek out programs that meet their specific needs. Programs like Charlie Mike, for example, provide emotional and social support to those living with the unseen wounds of combat.
As March is Brain Injury Awareness Month, it’s important to learn about these conditions and their effects on people everywhere. Keep your community informed on the devastating impacts of TBI, and remember to support the many veterans suffering from these injuries.
All wounds deserve to heal–even the ones we can’t see. Help a veteran heal today by donating to Charlie Mike. The proceeds help veterans access life-changing counseling, service dogs and equine therapy.




